In December 2017, when President Ram Nath Kovind warned of a potential “mental health epidemic” in India, it cast a light on one of India’s major public health concerns – and one of its most neglected. Mental affect significant numbers of Indians. However, mental health issues are often stigmatised in India, leading to many not seeking help.
“Our National Mental Health Survey, 2016 found that close to 14 percent of India’s population required active mental health interventions. About two percent suffered from severe mental disorders,” Kovind said at the time. Despite the findings, vast numbers of those suffering from mental health conditions remain undiagnosed. Of those with a diagnosis, few receive treatment.
“Invisible Illnesses” Still Yet To Be Accepted By The Public
The World Economic Forum cites India as having more than ten million children with autism, ten million people with epilepsy and more than 150 million people with a mental illness that will at some point require the intervention of therapy or other medical treatment. This number equates to just over ten percent of the population. Despite this, these “invisible illnesses” are often still stigmatised by the public.
At the highest levels, India is beginning to acknowledge mental health as a legitimate public health concern. More and more public bodies are beginning to acknowledge the concerns of the disabled and the mentally ill.
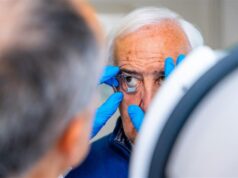
Parkinson’s Disease Is Scarcely Studied In India
The global average for Parkinson’s disease is roughly one percent in those aged over 65. As a degenerative condition it is found more commonly in the elderly, though early onset Parkinson’s disease does occur.
India suffers a clear drawback in assessing the extent it’s population is affected by the disease, it does not have official figures. This is a recurring theme for many mental illnesses and conditions. Particularly true of the more rare conditions, this fact alone may be denying many individuals of the treatments they need.
Crude prevalence rates have been established via door to door surveys in some area. One study found a rate of 14.1 per 100,000 amongst a population of 63,645 from rural Kashmir in the northern part of India. The prevalence rate over the age of sixty years was 247/100,000.
Parkinson’s Disease, India To Finally Receive Drugs Available Internationally?
Currently, Indian patients suffering from Parkinson’s disease struggle to access some of the more modern methods of treating the condition. This may soon change following the introduction of the drug Apomorphine, a treatment used commonly in Western nations.
Current treatments in India include the use of oral treatments, which come with the disadvantage of having diminishing returns once the disease begins to progress. Once Oral treatments are no longer effective, a far more intrusive process called deep brain stimulation (DBS) becomes necessary to alleviate the symptoms.
The potential availability of Apomorphine has many Indian neurologists excited. “Just one small dose of Apomorphine can bring substantial relief to the patients, and in India especially this drug will work wonders because not many can opt for the DBS procedure which is very expensive and in many cases, the other oral medications prove futile” says Dr. Girish Soni, professor of neurology at Sir JJ hospital.
Is Parkinson’s Disease A Good Representation Of The Situation For Other Mental Health Conditions?
In many ways the situation for Parkinson’s disease serves as an example of the current state of healthcare for mental illness in India.
The lack of nationwide data is an indication that the disease is neglected and left unstudied. For many in rural areas this can mean that they are never diagnosed as the disease is all but unheard of.
Access to medications is often limited, with those that are available being far less effective than what is currently being used in other nations. Government policy is in need of reforming to address the current mental health situation, while some bills have been put in place, their impact is debated.
The Mental Health Care Act 2017
The Mental Health Care Act 2017 replaced the older Act which has been in place since 1987. The old act was seen as outdated, and stigmatised mental health and infantilised those suffering from mental illnesses. The new act cements a number of rights for those suffering from mental illness.
These rights include: access to affordable health care (of which state hospitals are obliged to provide free of charge to those who cannot afford it), the capacity to provide informed consent and power to take decisions and the right of confidentiality and to live within a community.
Certain protections have been put in place such as the criminalisation of discriminatory behavior towards the mentally ill, as well as protection against intrusive procedures such as shock therapy.
Mental Health Care Act 2017 Dragging Its Feet On Insurance Coverage?
The Mental Health Care Act 2017 took the first steps in bridging the way for those suffering from mental illnesses to receive coverage under health insurance schemes. Despite this first step, many are asking whether progress is being made fast enough.
While free treatment is considered a right in state-run hospitals, many individuals may live so far from any state-run facility with the capacity to treat mental illness that they have little choice but to turn to the private sector. In these cases, insurance goes a long way in staving off crippling debt.
The act made it mandatory for health insurance companies to provide insurance to mental illnesses in the same manner they would for physical illnesses. Until recently, most insurance companies failed to comply with this provision of the act.
Without insurance coverage, treatment of mental health conditions can become an unmanageable expense. Bloomberg Quint gives the example of seventeen year old Akash. Akash suffers from bipolar disorder, often experiencing violent mood swings that have resulted in him occasionally having depressive episodes in which he considers taking his own life. These episodes would often result in prolonged — and expensive — hospital stays.
Akash’s family has so far spent over Rs 500,000 over the three years since his diagnosis. They say they were denied health insurance because counselling is an outpatient expense. Recognition and coverage under insurance policies are vital in ensuring adequate healthcare us provided.
Public Perception May Remain Unchanged For Some Time
Despite acknowledgements at a government level that there is an issue that so far has been largely unaddressed, real change will not occur until there is a large scale shift in public attitude as well as a considerable investment of resources by the government.
The attitude of the public may well take decades to address. Awareness campaigns may change the views of some but many may be entrenched in their views. It is therefore important that children are educated about mental health issues. Education from a young age regarding the rights and challenges faced by the mentally ill will improve awareness and could foster far more tolerant future generations.
Stigmatisation Is Still The Norm
The results of the report present a damning image. Of those surveyed only 27 percent said they would support someone perceived as having a mental illness. Almost as many (26 percent) claimed to actively fear the mentally ill.
Almost half (forty to 47 percent) claimed their awareness of the mentally ill was limited to stigmatised phrases such as “retard” and “mad”. 44 percent believed those with mental illnesses are always violent, while a further 41 percent believed interacting with the mentally ill can deteriorate the mental health of a healthy individual.
With views such as these being prevalent it is no wonder those with mental illnesses rarely seek help. Public attitudes need to change. Education is the key to this.
Developmental Disorders Are Prevalent Among India’s Youth
An assessment of 3,964 children between the ages of two and nine found almost an eighth suffer from at least one NDD (some may have several). Intellectual disabilities and hearing impairment disorders are the most common.
Depression Statistics Potentially Make India The “Most Depressed Nation”
In 2017 it was estimated that India held around 57 million individuals considered to have depression. There was no distinct correlation towards depression on a rural/urban basis, indicating the condition is just as common wherever you may live in India.
Depression can be caused by a myriad of factors. For some, it is a lifelong concern, for others, temporary. The cause may be a biochemical imbalance, it may be economic situation or the death of a loved one. The sheer number of causes make it a difficult situation to address without trained psychiatric staff, as therapy will ideally be tailored on an individual basis.
India’s lack of such staff means many of these individuals are all but on their own.
Loneliness And Depression In The Elderly
For some, loneliness is a contributing factor, nowhere is this more apparent than in India’s elderly citizens.
It is estimated that by the year 2020, approximately seventy percent of the world’s population aged sixty and above will be living in developing countries. 14.2 percent of them will live in India. Recent polling has shed new light on one of the most difficult issues facing India’s seniors: loneliness and depression.
Just one tenth of India’s seniors are not concerned about loneliness. 36 percent of those surveyed identified social interaction as their top priority in day-to-day life. This is per Juj Jug Jiyenge (“Live Longer”) – a survey of 1,000 elderly Indians across seven states conducted by IVH Senior Care, an elder care provider headquartered in Noida, Uttar Pradesh.
Mental illness is a significant issue when it comes to elders’ health concerns. Unfortunately, its significance is seldom recognised.
Data reveals that 21.9 percent of India’s elderly suffer from depression. This is a much higher rate than the global average. Fifteen percent of the world’s elderly population suffer from a mental disorder according to the World Health Organization (WHO).
The rise of depression among India’s seniors can be attributed to a number of reasons. As pointed out by the WHO, the elderly are vulnerable to a number of stressors which can trigger the onset of mental illness. These include illness, injury, a drop in economic status, and bereavement.
Ayurvedic Approaches To Treating Depression
Lack of treatment for mental illnesses is a considerable issue in India. Many areas may be almost entirely unequipped to deal with the issue. There is, however, evidence to suggest some ayurvedic practises may help alleviate some of the symptoms.
These traditional methods promote the use of music and dance movements in treating mental illness. Dr Sanyal claims that Indian classical music has different ragas which stimulate certain parts of our brain. This can have a therapeutic effect on the individual.
Such a simplistic method of treating often severe conditions such as depression warrants a considerable amount of doubt. However, some scientific studies back up these claims.
A review of a number of studies published on MentalHealth.org.nz shows that, in four of five studies investigating the use of music therapy in the treatment of depression, the outcome was positive. These studies were conducted by adding music therapy to the standard care routine of individuals suffering from depression. These results were then compared to a control group who were subject to only the standard therapy routine.
In four of the five studies it was found that levels of depression were reported by the subjects to be lower when they also received music therapy. The fifth study showed that on average the patients were reporting no significant change in mental state when music therapy was added to their treatment regime.
Suicide – The Extreme Final Result Of Mental Illness
Suicide is often a final resort of those suffering from mental illness, particularly issues such as depression. In India, the lack of mental health care and counselling services has left numerous groups committing suicide in vast numbers.
Farm workers are a group where this is seen in elevated rates. 36,332 farmer suicides occurred between 2014 and 2016. In that three-year window, 16,324 farm workers took their own lives.
The situation may in fact be getting worse for farm workers. Between 2015 and 2016, the number of farm workers actually dropped by 21 percent. However, farmhand suicides increased by ten percent.
Students are another group where suicide rates are far above average. More than one student commits suicide in the country every hour. This epidemic of mental health crises among India’s student population – projected to become the biggest in the world by 2025 – is one the country’s education system is ill-prepared to address, reports suggest.
If India is to address the situation a number of changes will need to be made, many of which may not be feasible within a short period of time. Public perception of mental illness needs to change, as the apathy or even revulsion of many members of the public drive many into secrecy or even to drastic measures such as suicide. Access to mental health services is also vital if those who suffer from these conditions are to get the help they need.
Dementia Incidence, A Future Crisis?
Worldwide numbers of dementia cases are estimated to hit 131.5 million by 2050.
India is unlikely to be exempt from this trend as conditions in the country indicate numbers are set to rise rapidly. India has an aging population, and with increased life expectancy in recent years the number of individuals living to the age of 65 and over is rising. Above this age the rate of dementia incidence increases at an almost exponential rate.
Two decades ago the condition was considered to be rare in India. However, current estimates place the number of patients with dementia in India at around 4 million. This may be a conservative estimate as countless numbers of people in rural communities may live with the condition without a diagnosis.
Lack Of A Cure Presents A Ticking Time Bomb Situation For India
India gained 2.9 million cases of dementia in 26 years according to recent research published in The Lancet. This trend is likely to continue, with the potential for this rate to increase as India’s population ages.
“Alzheimer’s carries with it significant economic and social costs. We need to intensify clinical research efforts to look for a cure for Alzheimer’s,” said Chirag Trivedi, President of Indian Society for Clinical Research.
Millions of sufferers in India warrant a vast number of carers to cope with the burden. Some may be able to afford residential homes for their dementia affected relatives. Many more still will need to care for their relatives themselves. This can become a 24-hour unpaid job as the disease progresses to the later stages and mental functions deteriorate.
This could have a considerable economic impact to India as a whole as swathes of the population may be forced to leave their jobs to care for elderly relatives. To the individuals themselves, such a matter could leave them in extreme poverty.
No Current Government Policies Geared Towards Dementia And Alzheimer’s Disease
India is entirely unprepared for a future in which the prevalence of Alzheimer’s disease rises sharply, according to the Alzheimer’s and Related disorders Society of India (ARDSI). There is currently no government policy put in place to address Alzheimer’s disease patients.
Without government intervention and established guidelines in addressing the rising numbers of those with dementia, India is all but entirely unprepared for the potential future in which many are forced into leaving the workforce to provide for elderly relatives.
Pollution And Dementia Risk
Urban air pollution is a key risk factor in developing dementia claims a study recently published in the BMJ Open. Does this finding suggest a future spike in dementia cases in India’s metropolises?
The study may shed some light on why Alzheimer’s disease is becoming more prevalent in India. Two decades ago it was a relatively rare condition. However, current estimates place the number of patients with Alzheimer’s disease in India at around four million. The relative rarity two decades ago may be due to lacking mental health awareness, though these new data suggest that the frequency of dementia and Alzheimer’s disease may indeed have been lower due to lower amounts of pollution.