
Vaccines will be offered free of charge to those aged eighteen and over, Prime Minister Narendra Modi has announced. The Prime Minister announced the free vaccines policy during an address to the nation yesterday, in which he stated “the Government of India itself will buy 75 percent of the total vaccine production from vaccine manufacturers and give it for free to the state governments.”
Modi billed the ongoing COVID-19 pandemic, which has seen a virulent resurgence in India in recent months, as the largest health crisis faced by the nation in a century. Such a proclamation seems apposite, especially given the challenges India is weathering.
The country has been particularly embattled by shortages of medical oxygen. As reported last month by Nicholas Parry for Health Issues India, many deaths during the second wave could have been averted were it not for the medical oxygen deficit. This issue has come under fire, with Allahabad High Court justices Siddhartha Varma and Ajit Kumar stating at a hearing “we are at pain in observing that death of COVID patients just for non-supply of oxygen to the hospitals is a criminal act and not less than a genocide by those who have been entrusted the task to ensure continuous procurement and supply chain of the liquid medical oxygen.”
This is not for want of supply. The problem is multifaceted. “The sudden surge of COVID infections and the subsequent need for supplemental oxygen in late March blindsided India’s health care network,” wrote Biman Mukherji for Fortune last month. “The country had assumed the worst of the pandemic was over. But within two weeks, the daily demand for medical oxygen spiked to twelve times pre-COVID levels, leaving hospitals like Batra struggling to treat the rush of patients who were showing up, gasping for breath.” It led to harrowing social media posts of individuals begging for oxygen. This is despite the fact that, as Mukherji notes in their analysis
“In truth, India always had enough oxygen. But as the second wave hit, it was being used for industrial—not medical—purposes. Ordinarily, India produces 9,000 tonnes of liquid oxygen each day. Only ten percent to fifteen percent of that goes toward medical supplies. The rest is used in industry, such as steelmaking. At the height of India’s second wave, which is still ongoing, COVID patients needed between 9,000 and 11,000 tons of oxygen. India had the capacity to meet that demand, but it would require diverting up to ninety percent of the country’s oxygen supply from industrial sites. Pulling that off took weeks—and government intervention.”
Vaccines too have been in short supply, in part due to a strategy of vaccine diplomacy embraced by the Centre which saw India export vaccine doses in their millions. To be more precise, on April 26th, Quartz reported that the country had exported 66 million vaccine doses. Since the onset of the second wave and the resultant chaos, a moratorium has been imposed on vaccine exports which has left a gaping hole in the global vaccination campaign. At home, vaccine shortages prompted palpable concern – and a volte face in the Government’s vaccine strategy as enshrined in Modi’s announcement of free vaccines for all over eighteen and a shift towards a more federalised approach.
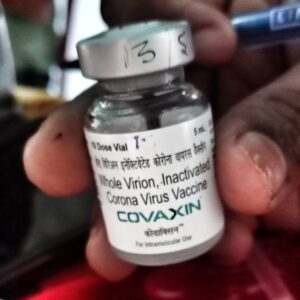
“Modi’s announcement on national television came after weeks of criticism of a bungled vaccine rollout that has covered fewer than five percent of India’s estimated adult population of 950 million,” Reuters summarised. “Health experts have warned that vaccination is the only way to protect lives from a third wave of infections after a surge in April-May overwhelmed hospitals in the big cities and in the vast hinterland.” On Sunday, the Government announced that almost 120 million vaccine doses will be available for domestic use this month versus the 79.4 million available in May.
Modi made a push in his speech for vaccine equity at home, stating “whether it is the poor, the lower middle class, the middle class, or the upper middle class, under the federal government programme, everyone will get free vaccines.” Federal coordination of the effort marks a transition from a more state-oriented distribution approach previously utilised. As Reuters explains, “under the earlier policy, the federal government gave free vaccines to the elderly and frontline workers, and left state governments and private hospitals to administer doses for a fee to people in the 18-45 age group.”
As Modi stated, “a lot of demands were raised that the states should get rights for their own COVID management. States demanded vaccine decentralisation, questions were raised on age group, on why senior citizens were vaccinated first. After giving it a lot of thought, we changed the way vaccinations were given. We thought to let the states monitor 25 percent of the vaccination work. It was given to the states on May 1. Within two weeks of May, some states started saying openly that the earlier system was good. More states joined in, even those who’d endorsed decentralisation.”
The scale of a vaccination programme in a country as populous and diverse as India has rarely, if ever, been overlooked. As Parry wrote for Health Issues India in December of last year
“India has had previous success stories stemming from vaccination. The prime example of this is polio, in which a concerted effort from the Government and grassroots coordinators saw a thorough immunisation campaign that culminated in the eradication of polio from the country. COVID-19 presents additional potential issues. The far more rapid spread of the condition could allow for the virus to have spiralled out of control through a second wave before a vaccine campaign has been fully implemented. The apparent necessity of a cold chain for the provision of the Pfizer vaccine in its current state could also mean that use of the vaccine in India’s isolated rural areas may be all but impossible. India’s vast population places it in a difficult spot amongst the global community in attempts to vaccinate against COVID-19. What is apparent is that in order to succeed, a herculean effort is in order.”
That second wave has come to pass in visceral terms, compounded by shortages of vital resources and a mismanaged vaccine rollout which is a far cry today from the peaks it enjoyed early on such as becoming the country to achieve four million inoculations in the shortest period of time. India’s COVID-19 crisis is one mammoth in scale, as is the effort needed to combat it. The announcement by Modi of free vaccines for all adults is heartening, but will require monumental, concerted efforts. In addition, it must be remembered that India – home to the world’s largest vaccine manufacturer and the so-called ‘pharmacy of the world’ – will continue to play an integral role in the global immunisation push even as it steps back at the moment.
The new policy has been welcomed. Reuters quotes Sudarshan Ballal, chairman at Manipal Hospitals, who said “the centre would have a lot more clout in dealing with the multinationals … rather than individual states or smaller players directly negotiating with these companies.” Concurring, Gautam Menon, professor of physics and biology at Ashoka University in Delhi, said the policy “eliminates states having to compete with one another for vaccine supplies, leaving them to concentrate on distributing them rapidly to their populations.”
The indication from the Prime Minister that India is recalibrating its strategy to curtail a pandemic which has claimed the lives of hundreds of thousands throughout the country is certainly welcome, though it must be remembered that the issues laid bare by COVID-19 are not new. Going forward, it is vital that the recalibration of the healthcare system to ensure the supply of medicines and equipment be foregrounded within the policy agenda. If and, likely, when the next pandemic comes upon us, we will suffer dearly if we do not learn the lessons from this tragedy.

