Tuberculosis (TB) presents a significant challenge to India’s healthcare system. Though political will to eliminate the condition is high, there are a number of hurdles that must be overcome to attain that goal.
Prevalence of tuberculosis
Estimating the true prevalence of the condition is difficult within India. The World Health Organization (WHO) reported last year that, of the ten million people who developed TB in 2017, 3.6 million were undiagnosed or their cases went unreported to the appropriate bodies. India was stated to account for a significant proportion of this gap. Alongside Indonesia and Nigeria, the country was responsible for eighty percent of unreported TB cases.
Issues typically arise where health centres — many of which are in the private sector — do not report TB cases. In Pune, for example, there are 6,771 registered healthcare facilities. Only 38 of them report cases of tuberculosis (TB).
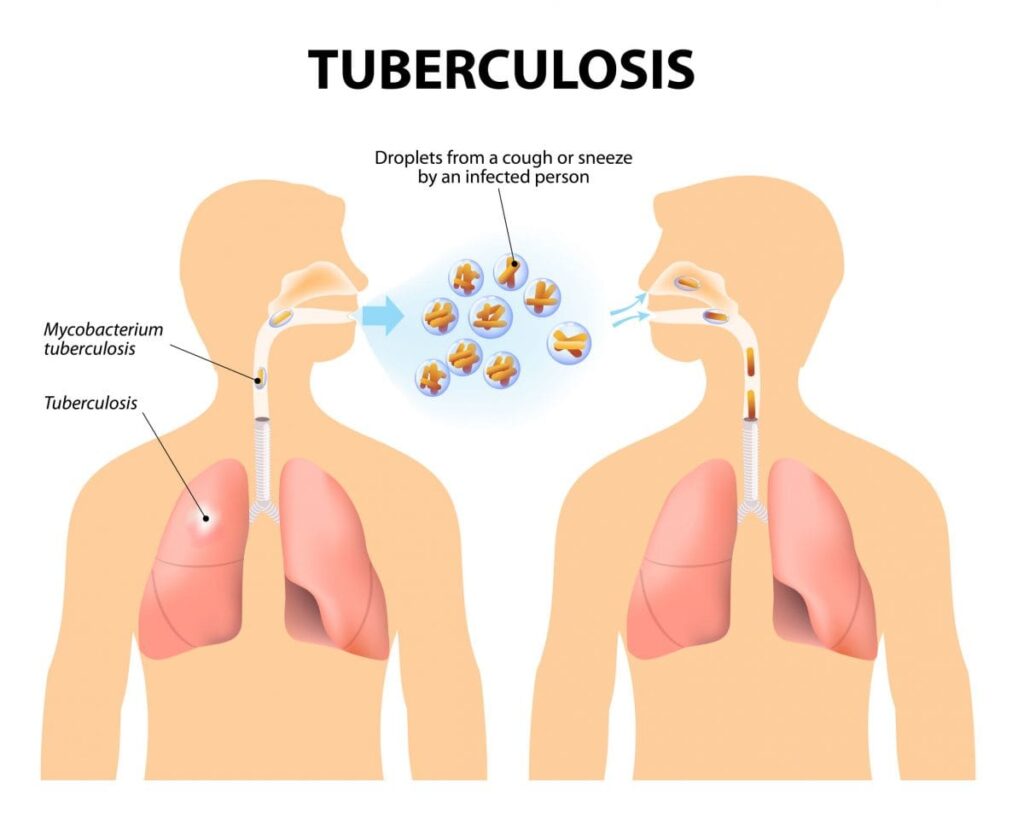
The condition is easily spread via droplets produced when coughing or sneezing, making it a highly contagious condition. Given the close proximity of individuals in India’s densely packed urban centres, there is ample opportunity for large-scale outbreaks of the condition.
Drug resistance
Development of drug resistance has presented a race against time to make the most of current medications before they almost inevitably become obsolete. Such an eventuality necessitates the use of the often far more expensive second-line therapies. Many of these are also being made less effective by the appearance of so-called “extensively drug-resistant TB” (XDR-TB).
Issues may arise regarding the supply chain. Whilst frontline therapies are relatively widely available, many second-line therapies or last resort therapies are available in only select places. Failure to supply these medications to areas with the greatest burden of TB could hinder efforts to eliminate the disease.
Bedaquiline, for example, has been hailed as a “miracle cure” in the treatment of XDR-TB. However, it is only available to a limited degree within India. Adding to the concern of the matter is that there are now reports from hospitals of bedaquiline-resistant strains appearing. Such strains, if widespread, could become all but untreatable.
Symptoms
A distinction is made between those who have “active TB” and “latent TB”. The latter occurs where an individual is harbouring TB bacterial cells in an inactive state, or one in which the immune system is preventing any forms of symptoms. In this state a person is not deemed contagious, though the condition can progress to active TB at any point.
The symptoms of TB closely echo that of the flu, making diagnosis an issue due to similarities with a host of other conditions. TB predominantly affects the lungs. Related symptoms typically involve coughing — which may last for around a month — as well as potentially coughing up blood. In this state the individual is highly contagious as droplets coughed out can infect others.
Other symptoms are flu-like and generic, including fever, fatigue, night sweats and chest pain. A lack of appetite may also occur, leading to unintentional and sometimes rapid weight loss.
Prevention and treatment
Preventing TB is difficult as the disease is so easily transmitted. Areas such as public transport or crowded areas are particularly prone to spreading the condition.
It is recommended, therefore, that if a person has been diagnosed that they isolate themselves as much as possible until they have finished their treatment regime. In this way they can minimise the exposure other people have and so reduce the risk of spreading the disease.
Tuberculosis is a treatable condition. Standard treatment procedures will include drugs such as Isoniazid, Rifampicin, Pyrazinamide and Ethambutol. In the case of drug resistance, one or more of these drugs are rendered ineffective and second-line therapies are necessary.


Great content great blog thanks for sharing follow Meddco Healthcare.
Please visit https://www.meddco.com/ for affordable packages